

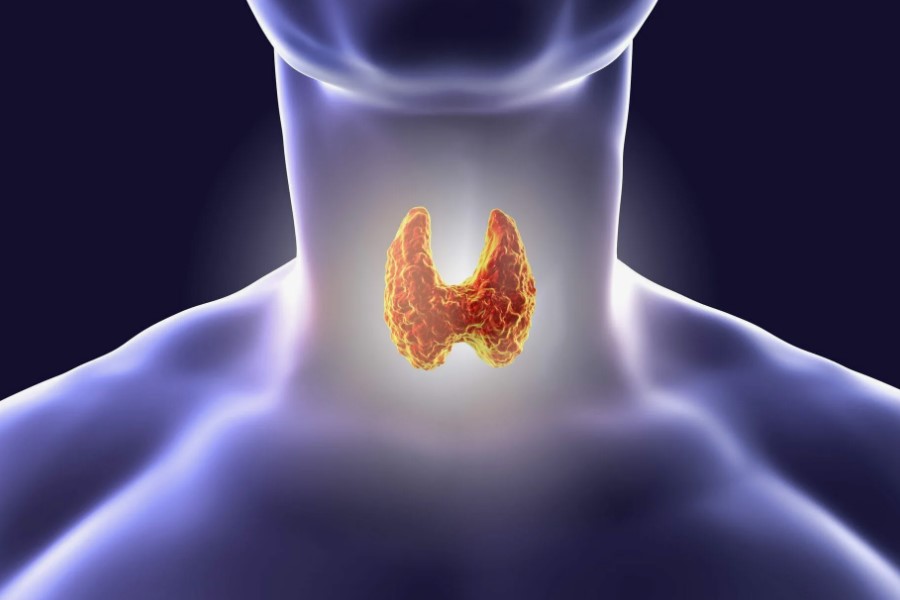
Parathyroidectomy The parathyroid glands are four small glands located behind the thyroid gland and are responsible for regulating blood calcium levels through parathyroid hormone secretion. This procedure is commonly performed to treat: Hyperparathyroidism Benign parathyroid tumors Chronic calcium imbalance disorders Goals of Neck Surgery: Safe removal of diseased tissue Preservation of vital neck structures, especially the recurrent laryngeal nerve Prevention of postoperative calcium deficiency Restoration of hormonal balance
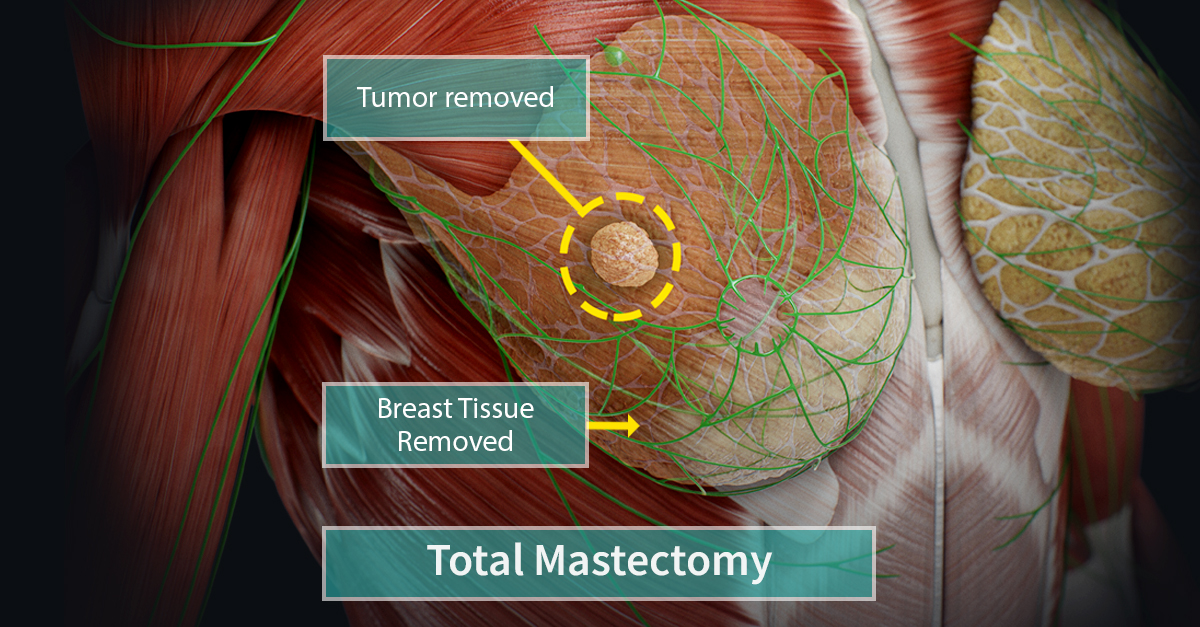
A mastectomy is a surgical procedure involving the removal of part or all of the breast tissue to treat or prevent breast cancer. Types of Mastectomy: Total (Simple) Mastectomy: Removal of the entire breast tissue while preserving the chest muscles. Modified Radical Mastectomy: Removal of the entire breast along with some axillary (underarm) lymph nodes. Skin-Sparing or Nipple-Sparing Mastectomy: Preservation of most of the breast skin (and sometimes the nipple) to facilitate reconstruction. Prophylactic Mastectomy: Preventive removal of the breast in high-risk patients. Partial Mastectomy (Lumpectomy): Removal of the tumor with a margin of healthy tissue. The choice of procedure depends on tumor size, stage, patient health status, and personal preference.
Conservative reconstruction aims to restore the natural shape and appearance of the breast after mastectomy while preserving as much healthy tissue as possible. It can be performed immediately during the same operation or delayed until after additional treatments (such as chemotherapy or radiotherapy). Reconstruction Methods: Implant-Based Reconstruction: Use of silicone or saline implants. Autologous Tissue Reconstruction (Flap Surgery): Use of the patient’s own tissue, often taken from the abdomen or back. Oncoplastic Techniques: Combining cancer removal with plastic surgery techniques to optimize cosmetic outcomes. Goals of Conservative Reconstruction: Achieve complete tumor removal. Maintain breast symmetry and natural contour. Reduce psychological impact. Improve overall quality of life.
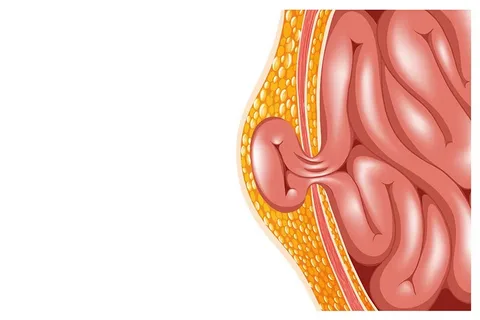
Inguinal hernia repair is a surgical procedure to fix a hernia occurring in the groin area. The surgeon returns the protruding tissue or intestine back into the abdomen and reinforces the weakened abdominal wall using a synthetic mesh. This reinforcement reduces the risk of recurrence and provides stronger support.
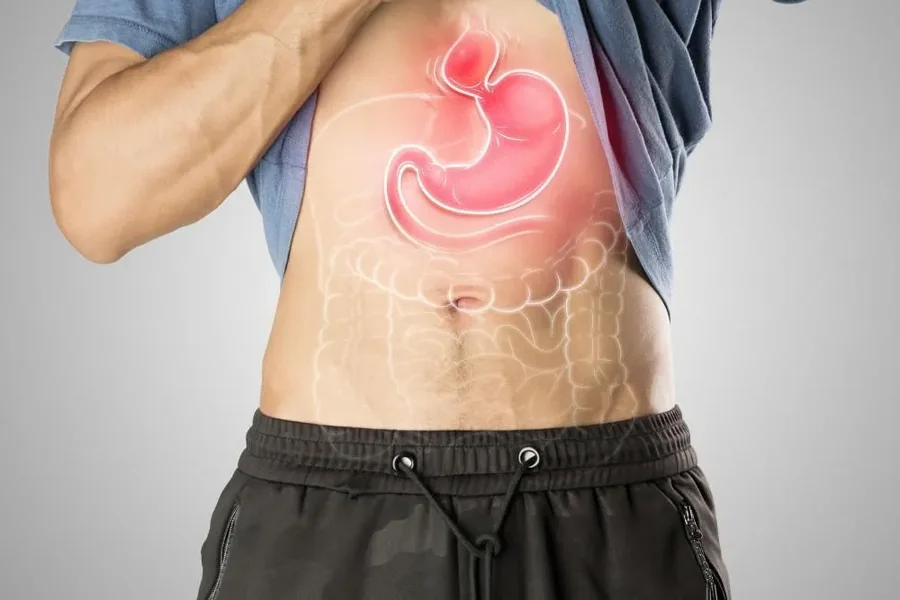
Hiatal hernia repair is a surgical procedure used to treat a hernia in which part of the stomach pushes up through the diaphragm into the chest cavity. The surgeon repositions the stomach into the abdomen and tightens the opening in the diaphragm. In many cases, the repair is reinforced with mesh to provide additional support. Laparoscopic surgery allows for faster recovery, reduced pain, and shorter hospital stay compared to open surgery.
Umbilical hernia repair is performed to treat a hernia near the belly button (navel). The surgeon pushes the protruding tissue back into the abdominal cavity and strengthens the abdominal wall with surgical mesh. Mesh reinforcement lowers recurrence rates and improves long-term outcomes.
Stomach Surgery These procedures address various gastric conditions, including tumors and severe ulcers. Gastrectomy: Partial or total removal of the stomach, commonly performed in cases of Gastric cancer. Gastric Ulcer: Severe or complicated ulcers (such as those causing bleeding or perforation) may require surgical intervention.
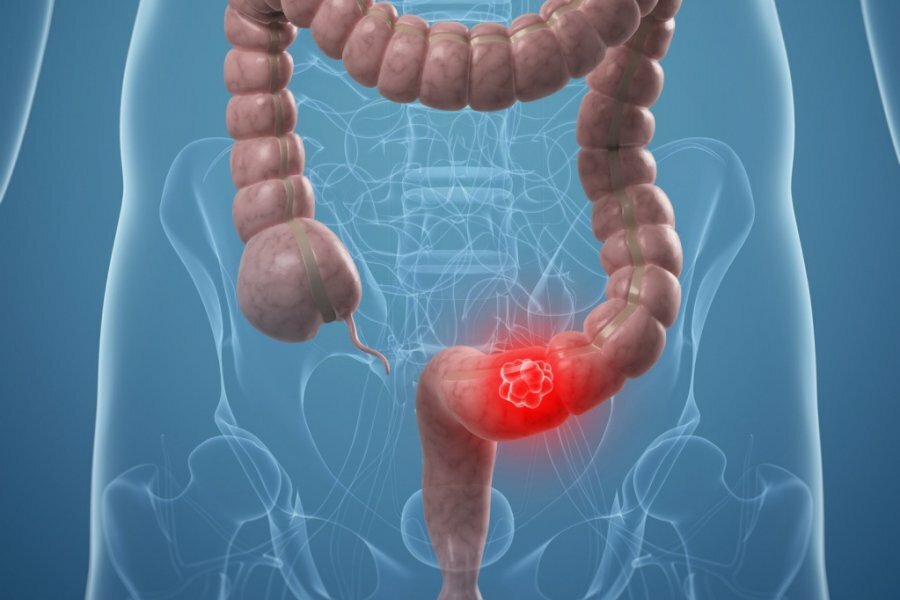
Right Hemicolectomy This procedure involves removal of the right side of the colon, including the cecum, ascending colon, and part of the transverse colon. Indications: Colon cancer affecting the right colon Large benign tumors Obstruction or severe bleeding Certain inflammatory conditions After removal, the small intestine is connected to the remaining portion of the colon to restore bowel continuity.
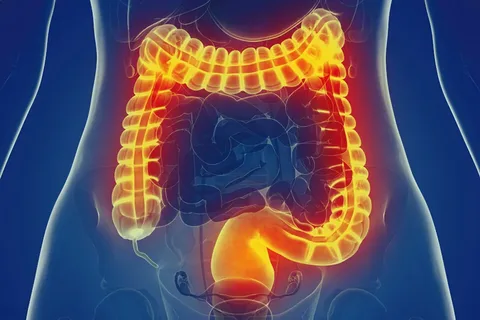
Left Hemicolectomy This surgery removes the left portion of the colon, including the descending colon and part of the transverse colon. Common reasons: Colon cancer on the left side Complications of Diverticulitis Bowel obstruction or significant bleeding The two remaining ends of the colon are reconnected to maintain digestive function.
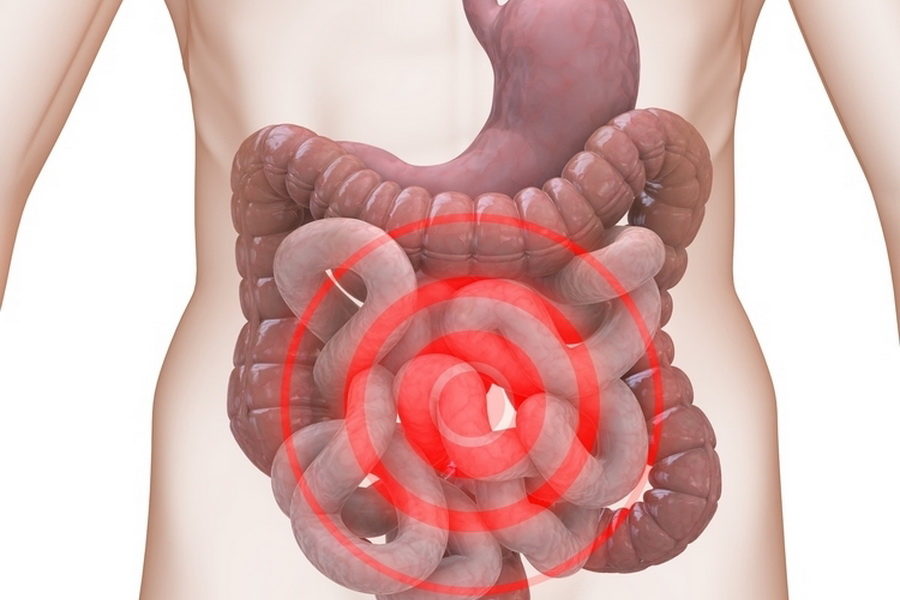
Sigmoid Colectomy A sigmoid colectomy involves removal of the sigmoid colon, the lower part of the large intestine near the rectum. Indications: Cancer of the sigmoid colon Recurrent diverticulitis Perforation or obstruction In some cases, a temporary or permanent colostomy may be required depending on the patient’s condition. Goals of Colon Surgery: Complete removal of diseased tissue Prevention of disease spread Relief of symptoms Preservation or restoration of normal bowel function
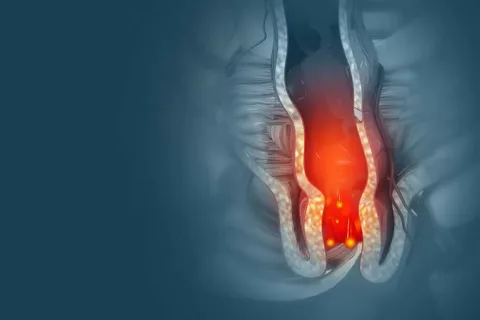
Hemorrhoids Hemorrhoids are swollen veins in the lower rectum or around the anus. Common symptoms: Bleeding during bowel movements Pain or itching Protruding lump Surgical treatment is considered in advanced or recurrent cases and may involve hemorrhoidectomy, ligation, or other minimally invasive techniques.
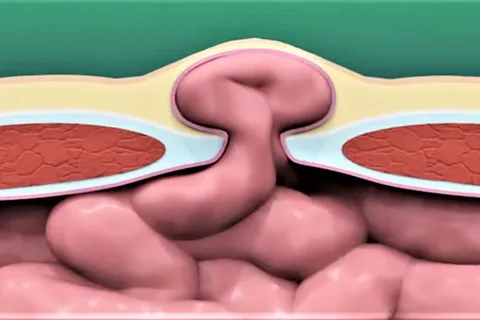
Anal Fissure An anal fissure is a small tear in the lining of the anal canal that causes severe pain, especially during and after bowel movements. While many cases respond to medications, chronic fissures may require a minor surgical procedure to relieve sphincter muscle spasm and promote healing.
Pilonidal Sinus A Pilonidal sinus is a chronic infection that typically occurs in the area between the buttocks due to hair growing under the skin. Surgical removal of the infected tissue is often required to prevent recurrence. Goals of Anal and Rectal Surgery: Relief of pain and bleeding Elimination of infection Prevention of recurrence Preservation of normal bowel control
Cholecystectomy Cholecystectomy is the surgical removal of the gallbladder, an organ that stores bile and releases it into the intestine to aid in fat digestion. Indications: Gallstones causing pain or inflammation Acute or chronic cholecystitis Obstruction of the bile duct due to stones Rare gallbladder tumors Surgical Approaches: Laparoscopic surgery: Minimally invasive, less pain, faster recovery. Open surgery: Used in emergencies or complicated cases.
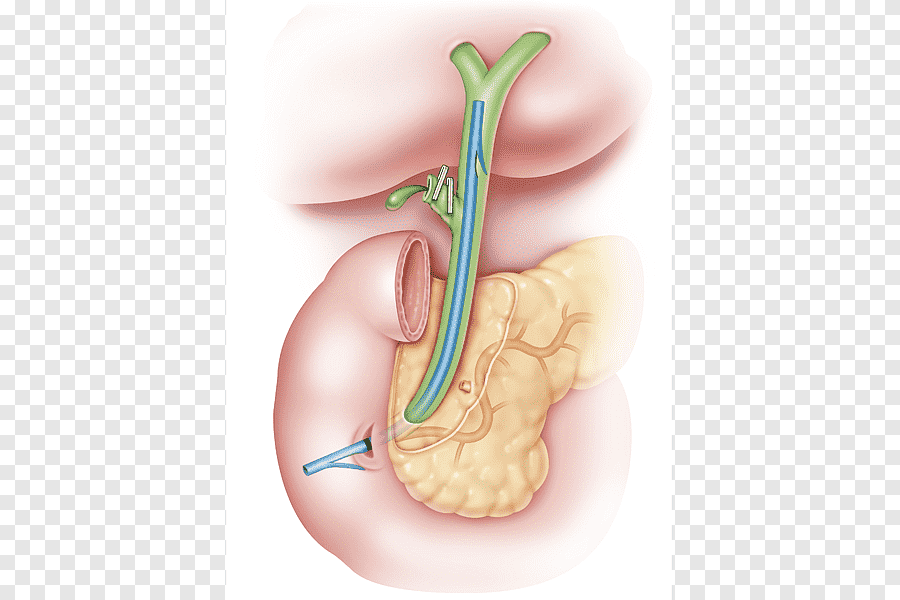
Common Bile Duct Exploration This procedure involves examining or opening the bile ducts to detect and remove stones or relieve obstruction, usually performed when bile flow is blocked or infection is suspected. Indications: Stones in the common bile duct Cholangitis Bile duct obstruction causing jaundice or infection Exploration can be done laparoscopically or through open surgery, depending on the patient’s condition. Goals of Liver and Gallbladder Surgery: Remove stones and prevent bile duct obstruction Treat infections and relieve pain Prevent serious complications like pancreatitis or jaundice Restore normal bile flow
Varicocele A varicocele is an abnormal enlargement of the veins within the scrotum, most commonly on the left side. It can cause discomfort and may affect fertility. Indications for Surgery: Chronic testicular pain Impaired sperm production or infertility Testicular enlargement or asymmetry Surgical Approaches: Open surgery: Ligation of the dilated veins to restore proper blood flow Laparoscopic or catheter-based procedures: Minimally invasive methods to correct varicoceles

Hydrocele A hydrocele is the accumulation of fluid around the testicle within the scrotum, usually painless but causing swelling. Indications for Surgery: Large hydrocele causing discomfort Complications such as infection or impaired mobility Persistent hydrocele with no spontaneous resolution Surgical Treatment: Hydrocelectomy: Removal of the sac and fluid to prevent recurrence Can be performed laparoscopically or via conventional open surgery depending on the size and condition Goals of Testicular Surgery: Relieve pain and discomfort Correct varicoceles to improve fertility Prevent complications from fluid accumulation Preserve normal testicular function
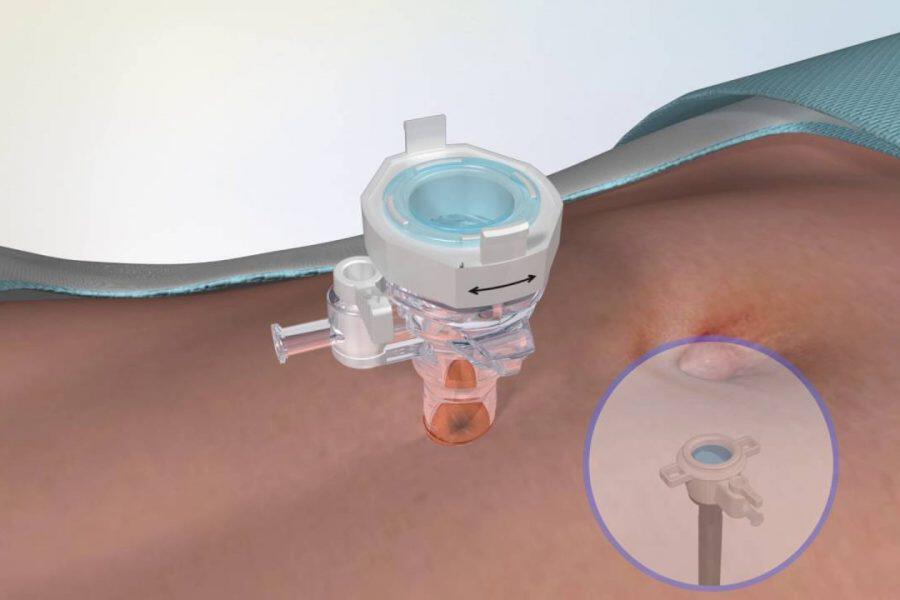
Laparoscopic inguinal hernia repair is a minimally invasive surgical procedure used to treat an inguinal hernia (a bulge in the groin area caused by weakness in the abdominal wall). Instead of a large incision, the surgeon makes small cuts in the abdomen and inserts a camera (laparoscope) and surgical instruments to repair the hernia. A synthetic mesh is usually placed to strengthen the abdominal wall and prevent recurrence. 🔹 What is an inguinal hernia? An inguinal hernia occurs when part of the intestine or fatty tissue pushes through a weak area in the lower abdominal wall, causing a swelling in the groin. 🔹 Advantages of laparoscopic surgery: Smaller incisions Less postoperative pain Faster recovery Shorter hospital stay Better cosmetic result 🔹 Recovery: Most patients go home the same day or next day Return to light activity within 1–2 weeks Avoid heavy lifting for about 4–6 weeks 🔹 Possible risks: Bleeding Infection Recurrence Injury to nearby structures (rare)

Laparoscopic umbilical hernia repair is a minimally invasive surgical procedure used to treat an umbilical hernia (a bulge near the belly button caused by weakness in the abdominal wall). Instead of a large incision, the surgeon makes small cuts in the abdomen and inserts a camera (laparoscope) and surgical instruments to repair the defect. A synthetic mesh is usually placed to strengthen the abdominal wall and reduce the risk of recurrence. 🔹 What is an umbilical hernia? An umbilical hernia occurs when part of the intestine or fatty tissue protrudes through a weak area near the navel, causing a visible swelling. 🔹 Advantages of laparoscopic surgery: Smaller incisions Less postoperative pain Faster recovery Lower infection risk Better cosmetic result 🔹 Recovery: Most patients go home the same day Return to normal activity within 1–2 weeks Avoid heavy lifting for 4–6 weeks 🔹 Possible risks: Bleeding Infection Recurrence Mesh-related complications (rare)
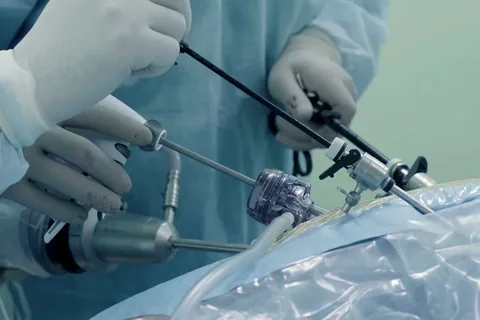
Laparoscopic hiatal hernia repair is a minimally invasive procedure used to treat a hiatal hernia (a condition where part of the stomach moves up into the chest through the diaphragm). Small incisions are made in the abdomen, and the stomach is repositioned into its normal place. The diaphragm opening is tightened, and sometimes an anti-reflux procedure is performed. 🔹 What is a hiatal hernia? It occurs when the upper part of the stomach pushes through the diaphragm into the chest, often causing acid reflux and heartburn. 🔹 Advantages: Less pain Short hospital stay Faster return to normal diet Minimal scarring 🔹 Recovery: Hospital stay usually 1–2 days Soft diet for a short period Return to normal activity within 2–3 weeks 🔹 Possible risks: Difficulty swallowing (temporary) Bleeding Infection Recurrence (rare)
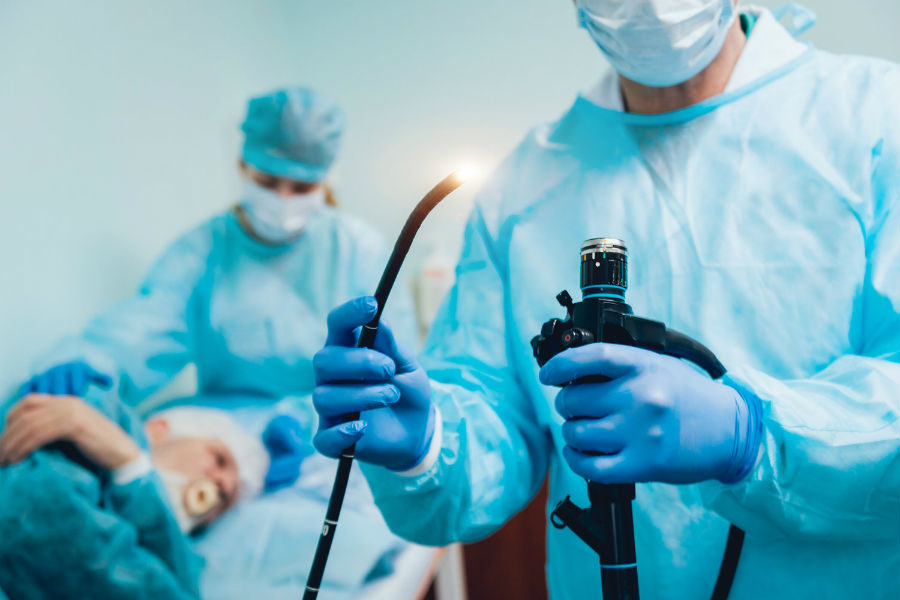
Sympathectomy is a surgical procedure that involves cutting, clipping, or removing part of the sympathetic nerve chain to reduce overactive nerve signals. It is commonly performed to treat conditions such as excessive sweating (hyperhidrosis), severe facial blushing, or certain pain and circulation disorders. The procedure is usually done using a minimally invasive technique called Endoscopic Thoracic Sympathectomy (ETS), where small incisions are made and a camera is used to guide the surgeon. This approach allows for less pain, minimal scarring, and faster recovery compared to open surgery.
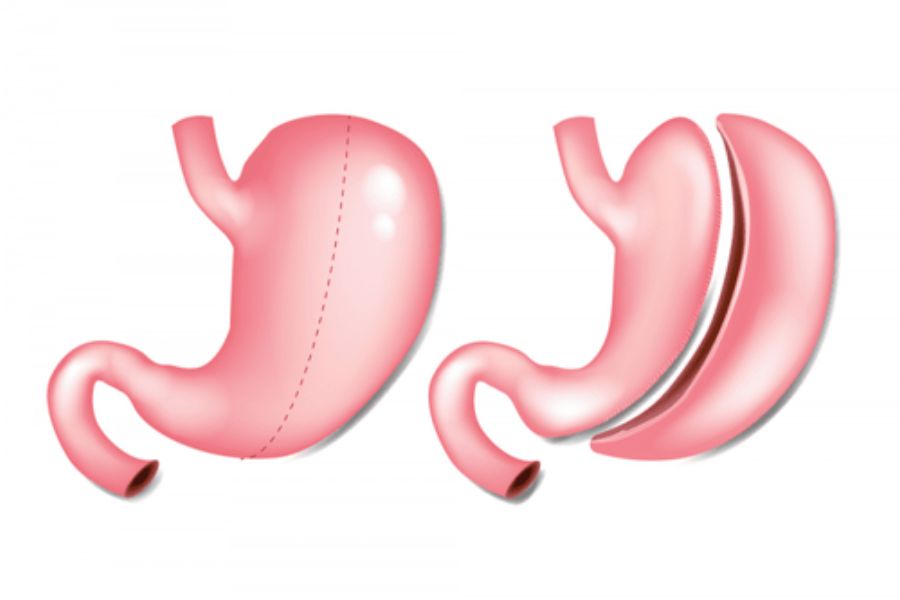
Laparoscopic gastrectomy is a minimally invasive surgery involving partial or total removal of the stomach, commonly performed for stomach tumors, severe ulcers, or weight-loss surgery. The affected portion of the stomach is removed, and the digestive tract is reconstructed. 🔹 Why is it done? Stomach cancer Complicated ulcers Bariatric surgery 🔹 Advantages: Less pain Shorter hospital stay Faster recovery 🔹 Recovery: Hospital stay 3–5 days Gradual diet progression Full recovery within several weeks 🔹 Possible risks: Bleeding Infection Leakage from surgical connection Nutritional deficiencies

Splenectomy is a surgical procedure to remove the spleen. It is performed to treat conditions such as splenic injury (trauma), certain blood disorders (like immune thrombocytopenia), enlarged spleen, cysts, tumors, or infections. The surgery can be done either through open surgery or laparoscopically (minimally invasive). In laparoscopic splenectomy, small incisions and a camera are used, resulting in less pain, smaller scars, shorter hospital stay, and faster recovery compared to open surgery. Since the spleen plays an important role in fighting infections, patients may need specific vaccinations before or after surgery to reduce the risk of infections.
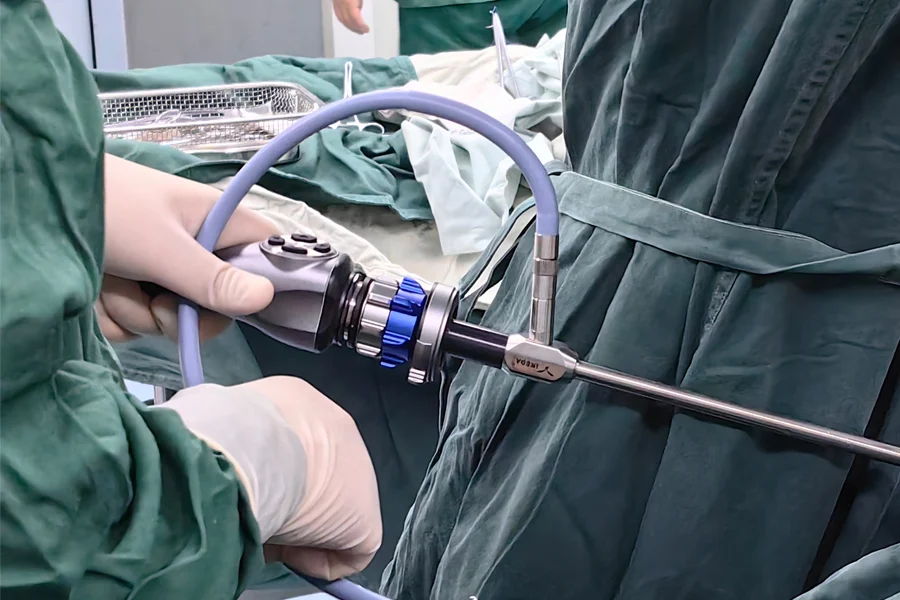
Diagnostic laparoscopy is a minimally invasive surgical procedure used to examine the organs inside the abdomen and pelvis. It is performed when imaging tests such as ultrasound or CT scan are inconclusive, or to evaluate unexplained abdominal pain, infections, tumors, internal bleeding, or infertility. During the procedure, small incisions are made in the abdomen, and a thin tube with a camera (laparoscope) is inserted to allow the surgeon to directly visualize the internal organs. If necessary, biopsies or minor surgical treatments can be performed at the same time. Laparoscopy offers advantages such as less postoperative pain, smaller scars, shorter hospital stay, and faster recovery compared to open exploratory surgery.
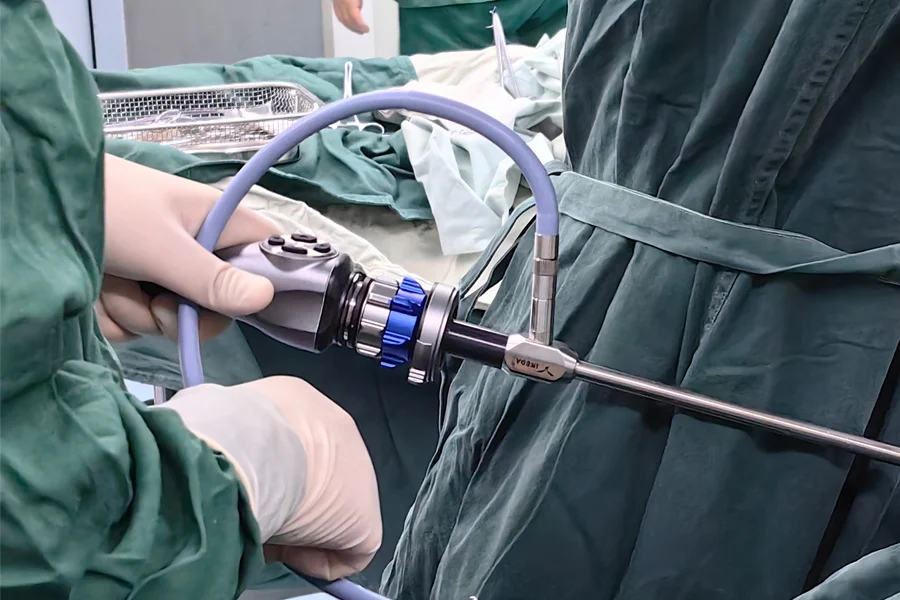
Laparoscopic varicocelectomy is a minimally invasive procedure used to treat varicocele (enlarged veins in the scrotum that may affect fertility). The surgeon seals the enlarged veins to improve blood flow and sperm quality. 🔹 What is varicocele? Enlargement of veins around the testicle, often causing infertility or discomfort. 🔹 Advantages: Small incisions Less postoperative pain Quick recovery 🔹 Recovery: Same-day discharge Return to normal activity within 1–2 weeks 🔹 Possible risks: Hydrocele formation Recurrence Infection