

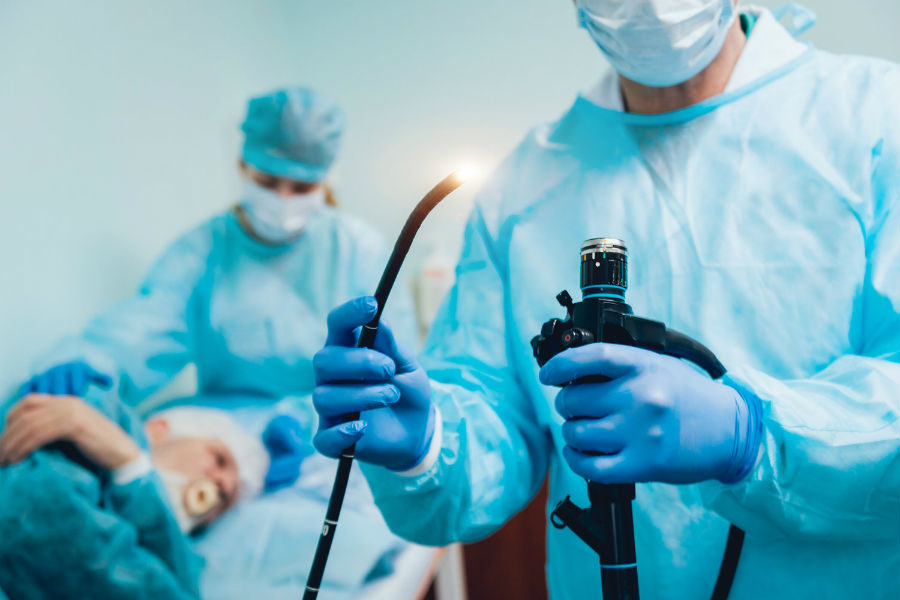
Laparoscopic inguinal hernia repair is a minimally invasive surgical procedure used to treat an inguinal hernia (a bulge in the groin area caused by weakness in the abdominal wall). Instead of a large incision, the surgeon makes small cuts in the abdomen and inserts a camera (laparoscope) and surgical instruments to repair the hernia. A synthetic mesh is usually placed to strengthen the abdominal wall and prevent recurrence. 🔹 What is an inguinal hernia? An inguinal hernia occurs when part of the intestine or fatty tissue pushes through a weak area in the lower abdominal wall, causing a swelling in the groin. 🔹 Advantages of laparoscopic surgery: Smaller incisions Less postoperative pain Faster recovery Shorter hospital stay Better cosmetic result 🔹 Recovery: Most patients go home the same day or next day Return to light activity within 1–2 weeks Avoid heavy lifting for about 4–6 weeks 🔹 Possible risks: Bleeding Infection Recurrence Injury to nearby structures (rare)

Laparoscopic umbilical hernia repair is a minimally invasive surgical procedure used to treat an umbilical hernia (a bulge near the belly button caused by weakness in the abdominal wall). Instead of a large incision, the surgeon makes small cuts in the abdomen and inserts a camera (laparoscope) and surgical instruments to repair the defect. A synthetic mesh is usually placed to strengthen the abdominal wall and reduce the risk of recurrence. 🔹 What is an umbilical hernia? An umbilical hernia occurs when part of the intestine or fatty tissue protrudes through a weak area near the navel, causing a visible swelling. 🔹 Advantages of laparoscopic surgery: Smaller incisions Less postoperative pain Faster recovery Lower infection risk Better cosmetic result 🔹 Recovery: Most patients go home the same day Return to normal activity within 1–2 weeks Avoid heavy lifting for 4–6 weeks 🔹 Possible risks: Bleeding Infection Recurrence Mesh-related complications (rare)
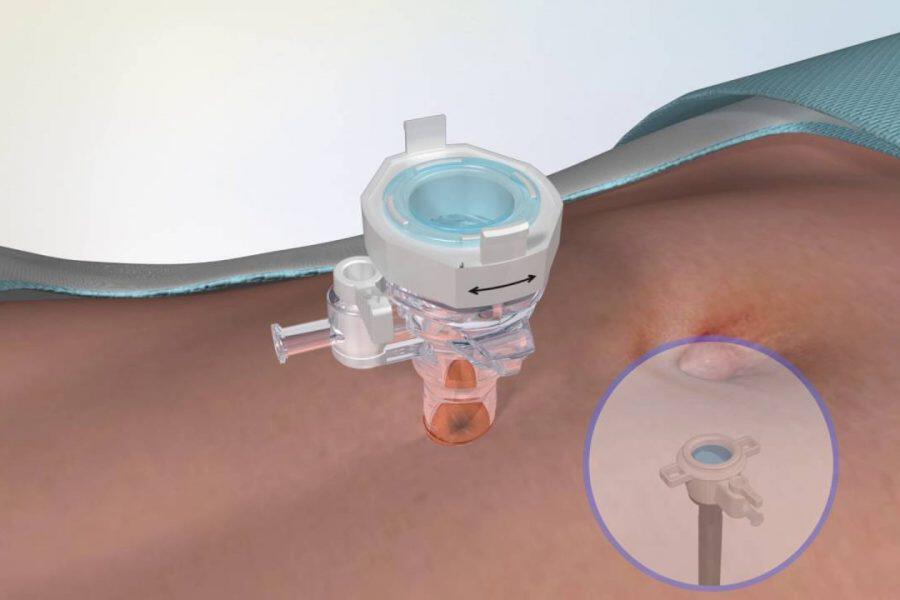
Laparoscopic hiatal hernia repair is a minimally invasive procedure used to treat a hiatal hernia (a condition where part of the stomach moves up into the chest through the diaphragm). Small incisions are made in the abdomen, and the stomach is repositioned into its normal place. The diaphragm opening is tightened, and sometimes an anti-reflux procedure is performed. 🔹 What is a hiatal hernia? It occurs when the upper part of the stomach pushes through the diaphragm into the chest, often causing acid reflux and heartburn. 🔹 Advantages: Less pain Short hospital stay Faster return to normal diet Minimal scarring 🔹 Recovery: Hospital stay usually 1–2 days Soft diet for a short period Return to normal activity within 2–3 weeks 🔹 Possible risks: Difficulty swallowing (temporary) Bleeding Infection Recurrence (rare)
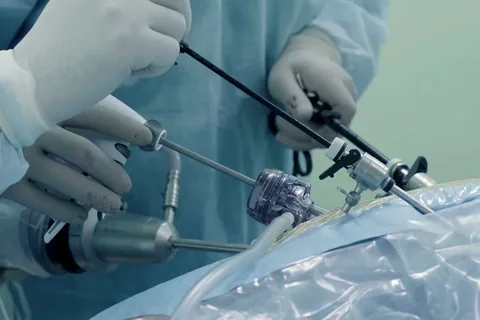
Sympathectomy is a surgical procedure that involves cutting, clipping, or removing part of the sympathetic nerve chain to reduce overactive nerve signals. It is commonly performed to treat conditions such as excessive sweating (hyperhidrosis), severe facial blushing, or certain pain and circulation disorders. The procedure is usually done using a minimally invasive technique called Endoscopic Thoracic Sympathectomy (ETS), where small incisions are made and a camera is used to guide the surgeon. This approach allows for less pain, minimal scarring, and faster recovery compared to open surgery.
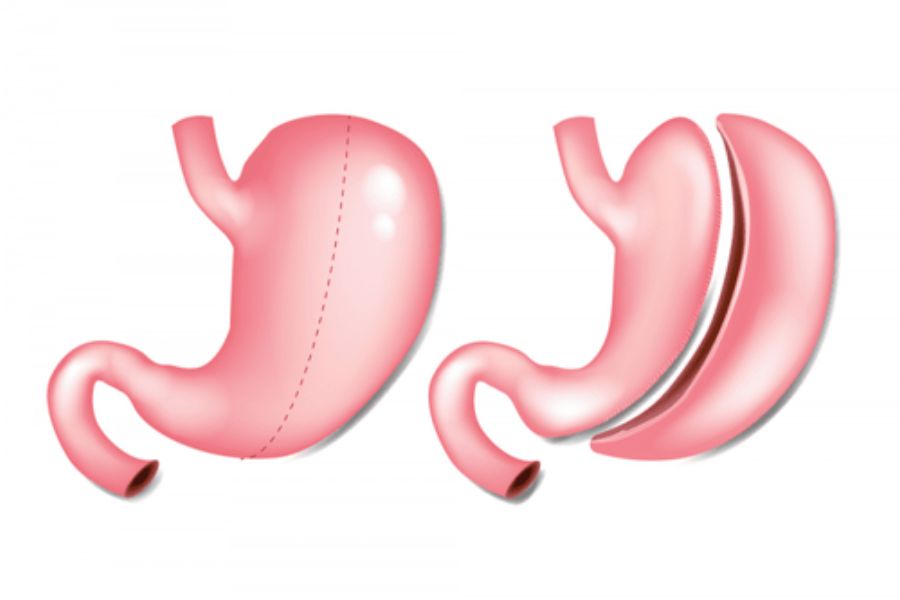
Laparoscopic gastrectomy is a minimally invasive surgery involving partial or total removal of the stomach, commonly performed for stomach tumors, severe ulcers, or weight-loss surgery. The affected portion of the stomach is removed, and the digestive tract is reconstructed. 🔹 Why is it done? Stomach cancer Complicated ulcers Bariatric surgery 🔹 Advantages: Less pain Shorter hospital stay Faster recovery 🔹 Recovery: Hospital stay 3–5 days Gradual diet progression Full recovery within several weeks 🔹 Possible risks: Bleeding Infection Leakage from surgical connection Nutritional deficiencies

Splenectomy is a surgical procedure to remove the spleen. It is performed to treat conditions such as splenic injury (trauma), certain blood disorders (like immune thrombocytopenia), enlarged spleen, cysts, tumors, or infections. The surgery can be done either through open surgery or laparoscopically (minimally invasive). In laparoscopic splenectomy, small incisions and a camera are used, resulting in less pain, smaller scars, shorter hospital stay, and faster recovery compared to open surgery. Since the spleen plays an important role in fighting infections, patients may need specific vaccinations before or after surgery to reduce the risk of infections.
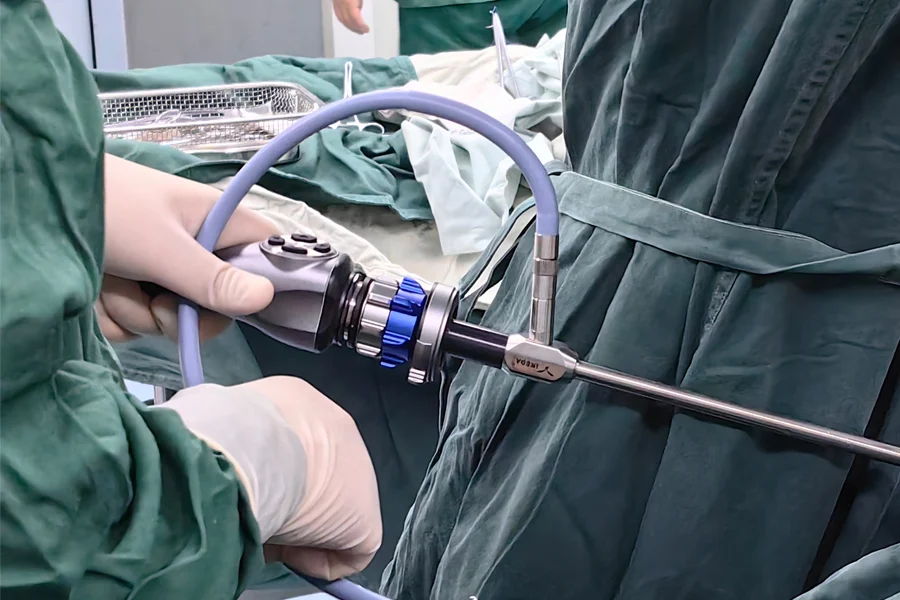
Diagnostic laparoscopy is a minimally invasive surgical procedure used to examine the organs inside the abdomen and pelvis. It is performed when imaging tests such as ultrasound or CT scan are inconclusive, or to evaluate unexplained abdominal pain, infections, tumors, internal bleeding, or infertility. During the procedure, small incisions are made in the abdomen, and a thin tube with a camera (laparoscope) is inserted to allow the surgeon to directly visualize the internal organs. If necessary, biopsies or minor surgical treatments can be performed at the same time. Laparoscopy offers advantages such as less postoperative pain, smaller scars, shorter hospital stay, and faster recovery compared to open exploratory surgery.
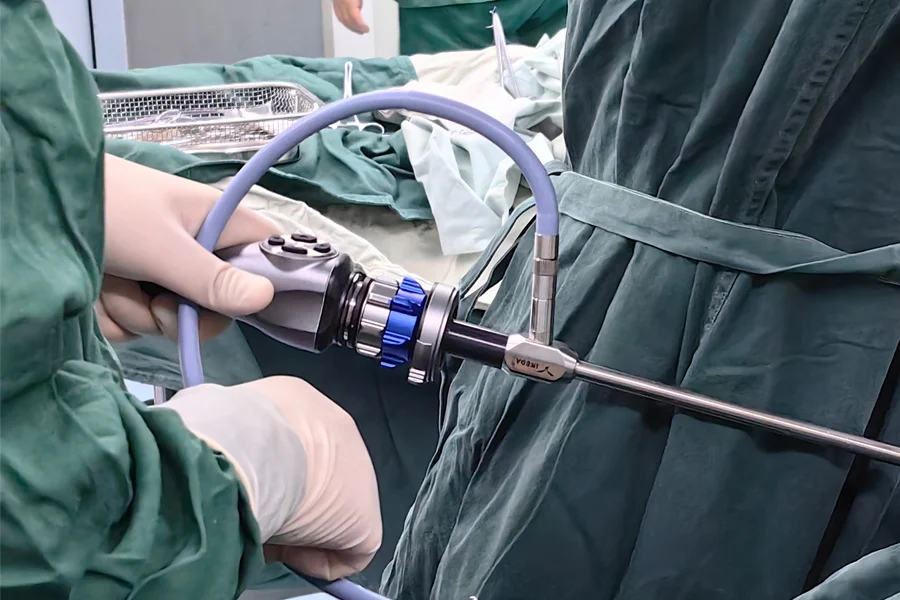
Laparoscopic varicocelectomy is a minimally invasive procedure used to treat varicocele (enlarged veins in the scrotum that may affect fertility). The surgeon seals the enlarged veins to improve blood flow and sperm quality. 🔹 What is varicocele? Enlargement of veins around the testicle, often causing infertility or discomfort. 🔹 Advantages: Small incisions Less postoperative pain Quick recovery 🔹 Recovery: Same-day discharge Return to normal activity within 1–2 weeks 🔹 Possible risks: Hydrocele formation Recurrence Infection